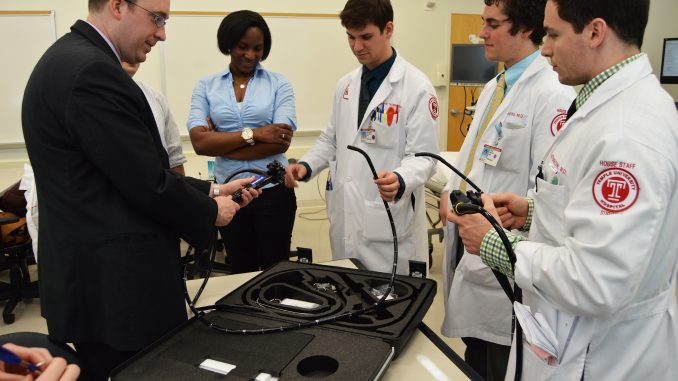
A new virtual reality simulator at Temple University School of Medicine alerts students when they’ve done something wrong – if a student makes a mistake during a mock colonoscopy procedure, the machine will emit a moaning or grunting sound.
The state-of-the-art training technology, called a Simbionix machine, provides in-depth training with upper endoscopy, colonoscopy and bronchoscopy procedures and comes with authentic scopes similar to those used in a medical office.
Students can insert one of the machine’s scopes into a designated procedure slot, and the camera at the tip of the long rubber scope allows the user to check a simulated patient for any irregularities, like Crohn’s disease, tumors and inflammation.
The program gives feedback on “how far you’re going in, if you’re hitting a wall, how fast you’re moving and more,” said Richard Milner, administrative director for the surgical research department.
The machine plays back the procedure in real time, so if mistakes were made, students can see what went wrong.
If the user were to make a mistake during a procedure, the machine generates a moaning or grunting sound, similar to one a patient would normally make.
Instructors can set the machine to different levels, and, using the scopes, students correctly diagnose the disease associated with the level.
All students have their own login to be used every time they need to perform a simulated procedure. The logins allow for recording a particular student’s improvement.
Dr. Matthew Philp is a colon and rectal physician at Temple University Hospital, as well as an assistant professor of clinical surgery at Temple’s medical school.
Philp leads the training sessions on the GI-BRONCH Mentor in the simulation lab.
A group of six surgical residents enter the lab at a time and take turns using the simulator within a three hour session.
Upon entering the room, each resident is instructed to take a preliminary skills assessment that questions their familiarity with equipment and procedures.
The point of the preliminary assessment is to gauge how useful the session is and to measure the effectiveness of the education, Philp said. As of now, use of the machine is recommended but not required, but Philp said that will change in a few years. He is designing a course around the machine, since it has the ability to boost students’ educational value by recording times and mistakes, he said.
The course will include “a graded system based on where they are and where they should be on the milestones we ask them to reach,” Philp said.
Dr. Deacon Lile is a surgical resident who used the simulated training technology. This was his first time doing a colonoscopy completely by himself, he said. He finds it’s harder to learn the “old way,” in which he said he had to learn “bit by bit” while shadowing a physician.
Before the machine, residents were allowed to perform certain parts of a procedure on a real patient. If a mistake occurred, a certified physician would take over, Lile said.
Lile said the simulator provides a less stressful environment.
“When there’s a patient on the table you get worried about harming them with every move you make,” Lile said.
Temple’s Institute for Clinical Simulation budgeted for the GI-BRONCH Mentor, which costs $160,000. It was approved in November 2014 but was first used in January of this year.
Milner pushed for this particular machine because it teaches the fundamentals of endoscopic surgery, he said. He describes it as a “didactic component in teaching hands on.”
“Simulation is a big part of our training nowadays,” Milner said.
Milner compares the simulator with the idea of how video games take real-life situations and put them on a screen.
“It’s like Halo,” Milner said, laughing. “Except you can skip levels.”
Jane Babian can be reached at jane.babian@temple.edu.


Be the first to comment